Service design in a rural California county brings insights into expanding the role of community-based organizations in Medicaid.
When paired with traditional health care, supportive services such as meal delivery and housing navigation can help reduce health disparities for high risk patients and improve health outcomes. Through 1115 demonstration waivers, states and CMS have begun to investigate coordinating health care, home- and community-based services, and supportive services within the Medicaid program. These services, funded as a way to head off more expensive medical interventions, are especially valuable for rural communities that struggle with access to health care services. Success in reducing health disparities will depend on recruiting community-based organizations (CBOs) and other providers that already serve focal populations for health equity.
In 2020, California started the CalAIM (California Advancing and Innovating Medi-Cal) Medicaid initiative aimed at improving health equity via coordinated, person-centered health and social services. Funded via demonstration, it’s one of the first of its kind in the nation.
CalAIM asks Managed Care Plans (MCPs) to recruit CBOs and other supportive service providers to supply 14 different types of supportive services, from housing navigation to medically tailored meals, to focal populations. Participating organizations in turn must integrate their systems with the existing Medi-Cal referral, billing, data exchange, and informed consent infrastructures. However, funding or staffing challenges may prevent providers from meeting increasing demand for services while simultaneously meshing their practices, culture, and staff with existing Medicaid infrastructure. How might CalAIM ensure that service providers get the support they need to meet the goals of an integrated approach to health care?

Known for its natural beauty and low cost of living, for decades rural Butte County was a haven for retirees—especially the town of Paradise. Wildfires, COVID, and skyrocketing housing costs have battered the community in recent years. Health services that were already stretched thin over a large area and isolated population have closed their doors. In a recent survey by the Butte County Health and Human Services Department, 34.1% of adult respondents reported having no primary health care provider.
Housing loss and displacement from the Camp Fire disproportionately affected those 65 and older, especially those who had lived in the town of Paradise, which the fire completely destroyed.
Geographic isolation is growing in rural communities. As well, there are fewer healthcare providers nearby, especially for the elderly. That means many groups are harder to reach through traditional health care providers.
In rural communities like those of Butte County, community-based organizations (CBOs):

This case study comes from A1M's ongoing partnership with a CBO in Butte County, where A1M is located. A1M supported the CBO as action-oriented researchers, donating company time and skills to help the director through the CalAIM enrollment process as a case study of rural Medicaid engagement. Activities included: attending webinars and regional CBO forums, interviewing shelter staff, and content analysis of publicly available documents and data from the State of California, MCPs, state vendors, and healthcare foundations.
One such CBO is the non-profit “Mountain Housing.”* For 25 years, it has run one of the largest homeless shelters in the county. As well, it also provides comprehensive navigational services, rapid rehousing, mental health support services, and street outreach. Many of its clients are Medicare and Medicaid beneficiaries, but the CBO has never gotten funding from either program.
Like many CBOs, Mountain Housing’s finances are perpetually shaky. Though successful with grants and local donations, it needs more reliable revenue to survive. Donations and sporadic grants can’t keep pace with rising demand in the aftermath of fire, displacement, and skyrocketing housing costs. “Tina,” its director, hopes that CalAIM will provide stable year-over-year revenue and support for adding new services that community members desperately need.
California is what’s called a “managed-care state,” which means that insurance companies are responsible for enrolling beneficiaries, processing claims, and making payments to providers. In the case of a demonstration like CalAIM, it is the Managed Care Plans (MCPs) that decide which of the 14 services to provide in each county, and which service providers will deliver each service. Before an organization can start providing CalAIM services, MCPs must also certify that any selected provider can fulfill all the Medicaid program requirements. There is no way to enroll without the active support of an MCP at every step.
When Tina starts the process of enrolling Mountain Housing in CalAIM in 2022, she doesn’t grasp the central role of MCPs. Based on her reading of the publicly available materials, she sees CalAIM as a state government program. As the director of a housing non-profit, she’s never interacted with health insurance companies. She reads through the program description on the state website, downloads the template for the application, and starts to fill it out, all entirely on her own.
Tina doesn’t know that other CBOs are having a more guided experience. Earlier, California had successfully run a precursor program to CalAIM in selected counties: the Whole Person Care pilot. California also ran focus groups with some CBOs in the run-up to CalAIM. CBOs engaged in the pilot or focus groups are more likely to have existing relationships with MCPs. As a result, CBOs from pilot counties have an accelerated, streamlined pathway to participation, and more understanding of how to work with health insurers.
Enrolling in CalAIM isn’t as simple as sending in an application. Understandably, organizations that are getting health care funding need to follow health care anti-fraud and patient privacy practices.
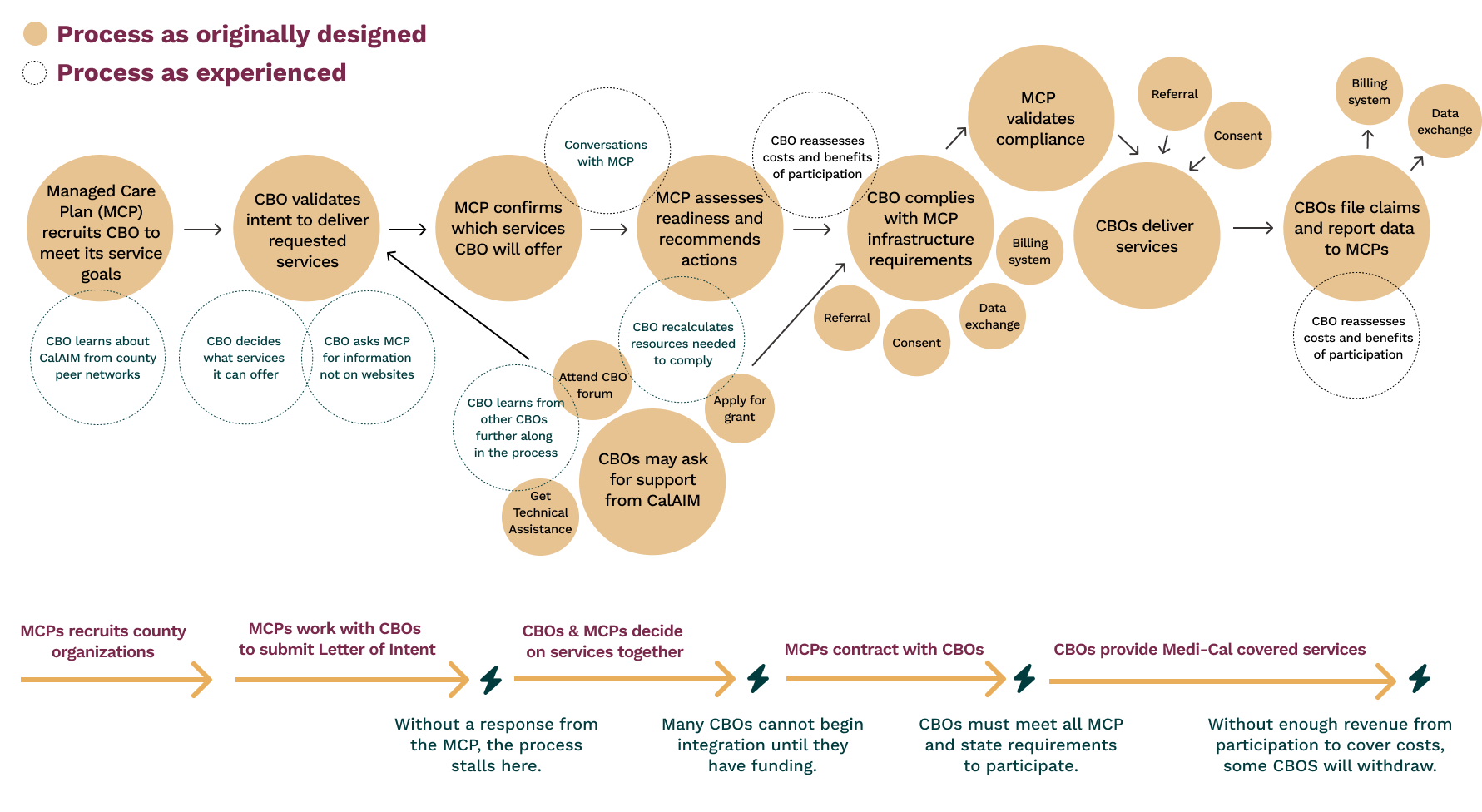
The image at the top of this section is a step-by-step visualization of both the official tasks (in orange) and the unofficial tasks at each of the steps required for CBOs to participate in California’s CalAIM program. As documented in official guidance, the process of enrolling in CalAIM (shown in the previous section) looks linear. What CBOs experience is more cyclical. They must repeatedly assess and reassess whether the benefit of participating is worth the large upfront investments it requires. For example, submitting claims requires both a HIPAA-compliant tool and trained personnel. To put them in place, a new provider will need funding and specialized technical assistance. To get funding and assistance, Tina needs to go through yet another uncertain application process.
At each step, Tina needs to get answers to three questions:

Answering those questions on her own is a challenge for Tina. She can find very little publicly available information about compliance costs, reimbursement rates, and typical denial figures, which she needs to prove to herself and the non-profit board that the investment of time and money is worth it. Personal contact with MCP representatives is required to complete the process — but Tina had trouble finding the right person. Meanwhile, the ongoing management crises of staffing and running an underfunded non-profit keep her from devoting regular time to the process during her work week. Instead, she sacrifices her Sundays to online research, data analysis, and follow-up emails.
Today, nine months after she discovered CalAIM, Tina has a signed agreement with her MCP to provide services. She found her MCP representative and established a positive personal relationship. But the biggest hurdles are yet to come. She still has to put in place (and pay for) the required infrastructure for treatment authorization, billing, and data exchange.
She’s learned a lot along the way, and so have we.
CBOs who had forged relationships with Managed Care Plans in pre-CalAIM pilots got access to unpublished information, especially about reimbursement, long before new-to-CalAIM providers like Tina.
There is a wealth of information about CalAIM’s goals and requirements available online. However, some of it is contradictory. No one document explains the whole process.
CalAIM represents a radical reimagining of community health. That means the housing- and food-oriented CBOs closest to hard-to-reach populations are unlikely to have Medicaid-standard billing tools and HIPAA-compliant systems, or prior experience implementing either. With extremely limited budgets, they may not be able to invest in compliance and administration without upfront support.
A1M is an approved technical assistance vendor for CalAIM providers, which means you can get help from us in enrolling and preparing for service delivery at no cost to you.

We embrace complex problems with a respect for the past and a vision for the future.